When I managed a unit that supported people who had dementia, I used to tell my staff that if someone’s behaviour suddenly changed and [for example] they became aggressive, they should always consider the ‘three P’s‘ first:
Piss (urine infection?)
Poo (constipation?)
Pain (generally)
…as these can all impact upon a person’s mental state, in particular people with dementia who are unable to articulate how they are feeling. If staff could rule these out first, they could often make huge difference to the quality of a person’s life, both physically & mentally.
I’ve not become aggressive, but in this and the next two blogs, I will be very personally & intimately discussing…
Piss, Poo & Pain.
If talking about these subjects already has you crying “too much information” then you really need to skip this entry altogether and the following two blogs (one for each ‘P’) and return when I get around to writing about normal stuff again.
In the style of the BBC News, before ‘Match of the Day‘,
‘if you don’t want to know the result, look away now‘.
Click here for some kittens, see you soon!
Right, now they’ve gone…
So you’ve acquired a disability?
Well, as they say, ‘shit happens’!
Except if you have a spinal injury, in which case, shit most certainly doesn’t happen
(at least, not properly!)
I’m a member of a few Facebook disability support groups. For people with spinal injuries generally and in particular, those caused by Cauda Equine Syndrome (CES), ‘Piss‘, ‘Poo‘ & ‘Pain‘ are regular subjects, especially with people who are new to their disability or simply, people who struggled alone for a long time before finding likeminded people. I’ve written repeatedly about my experiences which could offer some guidance to other people, but these are ‘private’ groups, and the ‘repeatedly‘ is a bit of a pain, so I decided to put it all here, then I can just link to these pages in future.
If you are coming here from one of the Facebook pages, I hope this information is useful. If you have further questions, feel free to email me; keith.fitton@outlook.com
I will separate the three P’s out in to individual blogs. This is number one of three.
[Edit August 2020: How was this not “number two’s of three”??? I’m losing my touch!]
Okay, I’m literally writing this blog while sitting in bed with a suppository up my bum, waiting for a rush to the toilet, where I will sit & shit for half an hour or so.
Yes, this is what you can expect from this blog… seriously, the kittens link earlier if offended, as it isn’t going to get any better!
But before we go any further:
DISCLAMER!!!
Some people will know I’m a Registered Nurse. THIS BLOG IS NOT MEDICAL ADVICE! I am intending to give some generalised advice regarding what has worked for me and how I have reached the ‘balances’ that I have. There may be things that you will try that work for yourself, in particular regarding neuropathic pain management. They may work, they may not, but they won’t do any harm. However, bowel & urine continence in particular should be discussed with a doctor or continence advisor. In the UK & Isle of Man, you should have access to a specialist continence advisor, who is generally a Registered Nurse. You may need a referral to a Urologist. Speak to your GP about such referrals. People in the USA or elsewhere, your systems are totally different, but discussion with a doctor, especially before making any major changes to bowel &/or bladder management is highly important. Simply making changes because ‘some bloke on the internet said so‘ is rarely a good way to manage health! But it may give you some ideas to discuss with the appropriate professionals, especially if your doctor isn’t familiar with these regimes.
First ‘P’… POO!
Or: ‘Constipation, What to do About It?‘
Or: ‘I Dare Not Go Out Because My Bowels Move at Random Times‘
Or: ‘Did you hear about the constipated mathematician? He worked it out using a pencil’
Almost everyone with a spinal injury experiences changes to the way their bowel works. Generally, people become constipated, sometimes impacted which is severe constipation. It is possible that this becomes a medical emergency. Sometimes people can be very constipated/impacted and experience very watery fluid being passed but no faeces. This is known as ‘overflow diarrhoea‘ or ‘faecal overflow‘. The ‘cure’ is to remove the hard stool that is causing a blockage, so it is important to understand that this isn’t regular diarrhoea. Also, for some people, they will finally clear a very large, often constipated stool, then get diarrhoea for a while afterwards.
This can be really disabling, often, as much as the inability to walk properly, because people are uncomfortable or in pain, stop enjoying food and daren’t go out or far from a toilet in case the bowel suddenly moves. They can’t plan anything because they don’t know what is happening. And they have the embarrassment of faecal incontinence. They can’t get on with ‘life‘.
Did I say “they“? I mean ‘we‘. I’ve had all of those in the past, including once shitting myself in a car with two friends present.
Oh the joy.
At least it was my car.
A bowel management regime now gives me the knowledge of when I will be evacuating my bowel and how.
I use a pattern based around ‘The Southport Regime‘. This is a regime to manage ‘neurogenic bowel dysfunction‘ which is what we call it if your bowel stops functioning normally after a spinal injury, including CES. It was initially devised at the Southport Spinal Injury Unit, an NHS service based (surprisingly enough) in Southport, England. The goal of the Southport Regime is to produce regular, “predictable” bowel movements that “takes less than an hour“, thus keeping the ‘intrusion‘ in to our lives, to a minimum.
Basically, the ‘Southport Regime‘ involves:
- Monday evening: Oral laxatives (senna tablets, lactulose etc)
- Tuesday morning: Suppositories
- Wednesday evening: Oral laxatives
- Thursday morning: Suppositories
- Friday evening: Oral laxatives
- Saturday morning: Suppositories
- Sunday, a day off!
It took me a bit of ‘playing around’ with the regime to find what worked best for me. Bearing in mind, I was working full time from December 2013 (having acquired my disability in May 2013) until November 2018, I needed a regime that worked consistently & predictably. I found that taking even eight senna tablets made absolutely no difference to me whatsoever. 10 ml of Lactulose syrup worked best for my oral aperient (‘softner’). Over time, I also settled on every other day, with no ‘day off’. I found that going three days (by skipping Sunday) the Monday stool was always more difficult to pass. However, this also means that if I have a specific reason, for example, if I have to travel early in the morning, I can ‘skip’ a day occasionally.
By planning ahead, I can insert some flexibility in to my routine by choosing when to insert a suppository.
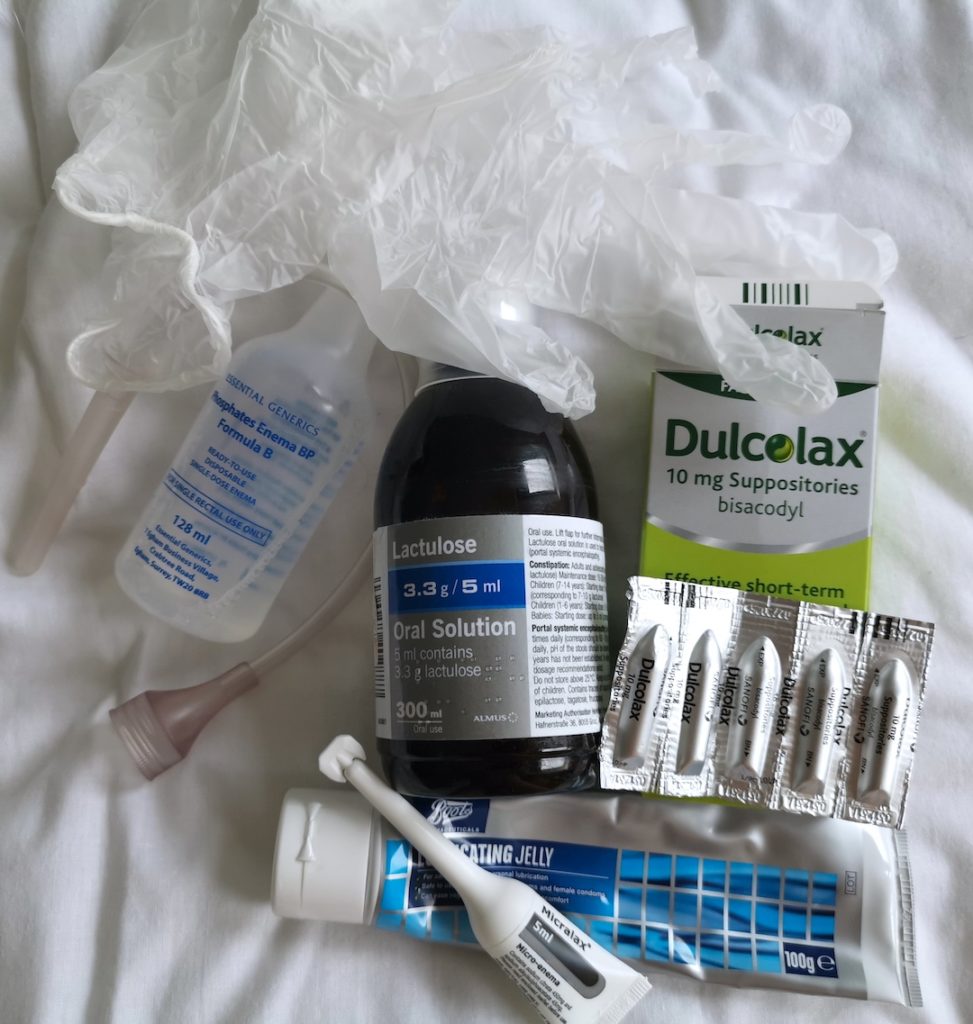
‘Microlax enema: For very hard stools (very rarely needed now)
Lactulose: Horrible, sticky, yucky. Softens the faeces.
Suppositories: Every other day.
Gloves: Obviously!
Lubricating Jelly: Be gentle! Just because you can’t feel anymore, doesn’t mean you won’t cause damage.
A bloke goes back to his doctor. He says “doctor, for all the good these suppositories have done me, I may as well have stuck them up my arse“…
Yes, suppositories go up your bum. They then melt and cause the bowel to move. The two main types of suppositories for bowel management are bisacodyl or glycerine. They work in slightly different ways. A doctor or specialist may suggest one or the other or even a combination of the two. Personally, I only use bisacodyl suppositories.
Enemas are another way of moving the bowel and some people use irrigation systems such as Peristeen, but they are different to what I’m talking about here. I would suggest discussing with your doctor or continence specialist, an approach such as Southport Regime first, then move on to other, more invasive approaches if needed. Obviously, some people will have been in rehab services etcetera where specialists skipped a regime such as Southport, because they can directly assess the damage to your spine.
This blog is aimed at people who don’t have a working system!
At the risk of labouring the point, this is guidance regarding what worked for me, speak to a professional who can assess you properly but there will be an answer if you look for it.
When I was working, I would wake up at 7am on “poo days”. Stick the suppository up while still in bed, then have a brew and surf Facebook or check email for about half an hour or so. I then would sit on the toilet and await an explosion.
Sometimes, I would have a massive torpedo fly out of my bum at warp speed! A foot long stool would be passed literally in a second! Due to a lack of sensation in that area, I wouldn’t feel it being passed but the sudden ejection would leave me feeling a bit sick further up my bowel. This feeling would be weirdly satisfying! Not at all pleasant, but ‘satisfying‘. I would tend to sit for a while longer, but rarely pass anything else.
On other occasions, it would be difficult to get going. I may have to sit for a while before gravity helped. I would sometimes have to strain. THIS IS NOT RECOMMENDED! But, sometimes it is needed. Occasionally, I would have a push, then stand up and holding some tissue against my anus, ‘palpate’ up and down. I would then sit back down and push all in one go. Very rarely, I would need to ‘manually evacuate‘ by inserting a finger.
This needs to be done very, VERY, VERY gently!
Due to a lack of sensation in the area, it is much easier for someone with a spinal injury to cause damage without realising it.
Again, discuss with a professional.
The point is, even with a well managed bowel routine, there may still be changes in consistency and response. Diet is a huge influence. A high fibre diet, with lots of fruit & vegetables will lead to a healthier bowel and easier movement as well as a healthier lifestyle generally. My wife & I are trying, generally unsuccessfully, to have at least two vegetarian days every week. When we achieve this goal, I notice a difference in bowel movements. Also, exercise can make a big difference. Depending upon the type of injury you have will impact upon how easy or difficult it is to take part in exercise, but anything that you can do will be useful. My main exercise is wheelchair basketball which I blogged about previously. It is very easy to fall in to a cycle of unhealthy living after acquiring a disability… less exercise & more isolation leading to eating less healthy food, more junk food or ready meals because they are easier, leading to feeling depressed so eating more cake and crap etcetera, etcetera, etcetera. These all change the way an already dysfunctional bowel works… or doesn’t. Likewise, worrying that you may be incontinent while out and about leads to becoming more socially isolated, again leading to depression, further withdrawal and again, more unhealthy lifestyle. It is a vicious circle, where life is limited, not by the injury to the spine, but because life revolves around bowels.
Establishing a good bowel routine took me a little while with some trial and error. I’d recommend making small changes to laxatives etc rather than changing everything all in one go. When I was in rehab, I was taking Laxido, which is a laxative that comes in powder form, which is added to water to make a disgusting tasting concoction. I found that this was too vicious.

Likewise, senna tablets made no difference whatsoever. If I’ve been good and eaten a lot of vegetables with little or no meat, I will skip the Lactulose for a night. Generally though 10ml Lactulose at night and a 10mg bisacodyl suppository the following morning does the job.
Get to know your own body.
Tweak the regime as needed. The point I’m trying to make is, I have a well established bowel regime but I don’t do exactly the same thing day after day. So if my regime still occasionally requires tweaking, then there isn’t a ‘one size fits all‘ for everyone reading this. But there will be ‘something‘ that works and gives you hope. If you are reading this because you are having difficulties around constipation or faecal incontinence, then hopefully this will give you some pointers as to where to begin regaining control. Speaking to a professional is the starting point, but ask them questions. Be an ‘informed patient‘. It may be that you need more active intervention, such as enemas or irrigation systems. But the important thing to know it that there are answers and you can regain control.
If you’ve any questions, feel free to email me: keith.fitton@outlook.com
And if you came from a Facebook group directly to this page, if this was useful (or even just made you smile) please leave a comment and visit the main ‘landing page’ www.rollingwith.me so that you can subscribe for future updates. Perhaps you’ll enjoy reading the previous entries too?
The next two blog entries will cover ‘Pee’ & ‘Pain’.
Fun Fact for American Readers:
Words like ‘faeces‘ & ‘colour‘ are spelt differently over there, in part because of cost! In the USA, type setters were paid by the letter, so newspaper owners dropped the ‘superfluous letters‘ to make it cheaper to print news.
Also, at the time, there were inconsistencies in English spelling, even in England. There still are. For example, most Brits will write ‘realise‘ not ‘realize‘, even though both are correct. Across the pond, in 1828 ‘Webster’ developed the first US dictionary, in an attempt to standardise (or ‘standardize‘ as Webster would prefer) spelling throughout The New World.
While many of us bemoan those in the colonies ‘dumbing down‘ of our language, in fact, we’ve adopted some of Webster back over this way. For example, prior to 1828, words like ‘music’ were generally spelt ‘musick‘. As well as the ‘U’ in colour, which we desperately cling to, Webster removed the ‘K’ from ‘publick‘ which we accepted. Funny old world.
So returning to the subject;
If you want to soften the faeces, you should get with the programme & centre in on a high fibre diet!


