I’ve mentioned in a previous blog, how changing the way you respond to a simple question can make a massive difference to your mental health. When still in hospital after acquiring my disability, I realised that if people asked ‘how are you?’ then the answer, compared to not long before, when I could walk, was always going to be ‘a bit crap really‘. Instead, when asked, I began to deliberately remember my ‘lowest point‘, my first physiotherapy session. Then the answer became ‘really good‘, as I focussed on the positives, not the negative.
My ‘other lowest point‘, possibly, if truth be told, even lower point than the physiotherapy session, was while in rehab.
Cauda Equina Syndrome (CES) manages to cause both urine incontinence (peeing uncontrolled) and urine retention (being unable to pass urine). Great, a full bladder that won’t empty when you want it to and a bladder that will allow urine to pass when you don’t want it to… What a joy!
I’d not long had my indwelling catheter removed and had moved to a system called Intermittent Self Catheterisation (ISC). I’ll come back to this later, but for now, sticking to that lowest of the low points…
I was laying on the bed in the rehab unit, ready to ISC in order to empty my retained bladder. The catheter got ‘stuck’ as it was entering the bladder itself, as it hit the tightly shut sphincter muscle. This caused ‘trauma’ to the sphincter (I assume).
The catheter tube filled with bright red blood.
At the same time, urine shot through the now forced open muscle, down the OUTSIDE of the catheter, causing a fountain of pee to spray in to the air, then all over me and the bed!
In anger & frustration I threw the blood filled, pissed wet through, catheter & bag across the room, but with the sphincter forced open, the fountain of pee continued until the pressure in my bladder dropped enough for it to re-seal.
I lay in the wet for a few moments while I composed myself.
Then after a deep breath, I showered & changed, before stripping & remaking my bed. This was no mean feat, I was still 100% a wheelchair user at the time but I’m a stubborn git and I wasn’t having anyone else cleaning up after me!
If you found this blog because you Googled “golden shower” this probably isn’t what you were expecting!
And if you didn’t get that joke, I suggest you Google Images for “golden showers“… best not to do so from work computers though.
Go on, we’ll wait for you…
Hmm, they’ve been a while, perhaps they aren’t coming back? Ah well, each to their own…
As with the first of the ‘Three P’s Series‘, this one will have some people already retching and thinking ‘too much information‘. If that’s you, here’s some puppies playing, as it won’t be getting any better than this.
As with the bowels blog, here is a very important bit to read & understand:
Disclamer.
Some people will know I’m a Registered Nurse. THIS BLOG IS NOT MEDICAL ADVICE! I am intending to give some generalised advice regarding what has worked for me and how I have reached the ‘balances’ that I have. There may be things that you will try that work for yourself, in particular regarding neuropathic pain management (next blog). They may work, they may not, but they won’t do any harm.
However, bowel & urine continence in particular should be discussed with a doctor or continence advisor.
In the UK & Isle of Man, you should have access to a specialist continence advisor, who is generally a Registered Nurse. You may need a referral to a Urologist. Speak to your GP about such referrals. People in the USA or elsewhere, your systems are totally different, but discussion with a doctor, especially before making any major changes to bowel &/or bladder management is highly important. Simply making changes because ‘some bloke on the internet said so‘ is rarely a good way to manage health! But it may give you some ideas & pointers to discuss with the appropriate professionals, especially if your doctor isn’t familiar with these regimes.
Okay, now we’ve got rid of the readers who have a weak stomach and I’ve done enough to not get sued, we can get down to talking about ‘passing urine’ or ‘peeing’.
Let’s go back to the ‘low point‘ story above. Having pissed all over myself and the bed, showered and changed, I still had a pretty full bladder. I sat on the toilet and leaning forwards, with a hand pushed against my bladder, I found that urine was passed. I kind of ‘rocked’ backwards and forwards, with urine coming out in squirts, almost like milking a cow by hand, as the teat was pulled, milk came out, as I rocked and pushed, pee flowed.
I had unknowingly stumbled upon ‘The Crede’s Method‘ of emptying my bladder. I never returned to ISC.
But ISC remains the preferred approach to bladder management, and for good reason. And indwelling catheters are something everyone who acquires a disability due to a spine injury will have experienced, so let’s start there.
Catheters:
For urine output, there are basically four types of catheters.
- Urethral indwelling.
- Suprapubic (SPC) indwelling
- Intermittent Self-Catheterised (ISC)
- Male conveen
A conveen is like a condom with a connector to attach to a urine leg bag. It is sticky on the inside, so as it unrolls on to the penis, it sticks to the skin. There are two important things to remember when applying a conveen. Firstly keep pubic hair trimmed, because hair can allow urine to track in to the conveen and it will leak. Secondly get plenty of warmth in to the conveen when applying it, as this will make the glue stick better.

The biggest advantage with conveens is that you are very unlikely to get an infection. The biggest disadvantage is that they can come off and/or leak. Also, if you have a spinal injury resulting in retention then you aren’t going to get any advantage from a conveen as the retention will remain. The other key disadvantage with a conveen system is that you need a penis, so if you haven’t got one of those, you are out of luck. If you are a bloke who is incontinent due to a condition such as MS then a conveen may be a good way to manage your condition.
Of the two indwelling catheters, a urethral catheter is the most common. Basically, a tube is inserted in to the urethra, which is where urine comes down normally. Once in the bladder, a small balloon is filled with water. This then stops the catheter from coming back out again. Urine then drains through the catheter and in to a leg bag. The bag has a tap on the bottom, so it can be emptied. Generally, a larger bag is attached at night time, so that it doesn’t need emptying while you are asleep.
The biggest problem with this type of catheter being used on a long term basis is that you will get infections. Not ‘if’ but ‘when‘. In effect, you are supplying bacteria with a nice ladder to head from the outside world straight in to the bladder. Good hygiene will reduce the infections, but it will happen if used long term. Ladies, having a smaller urethra, therefore a shorter ‘ladder’, are likely to get more infections than men, but it will happen to everyone at some point. Some people may even require a regular ‘prophylactic’ [‘preventative‘] dose of antibiotic, which is yet another drug to take.
Other problems are that they can be uncomfortable, although most of us have decreased sensation in that area, especially those of us with CES, so less of an issue in that case. The pipe can also become kinked, which stops the urine flowing or the ‘eyelet’ at the top of the catheter can become blocked. Either of these will cause the urine to back-up as the bladder fills, until the pressure forces urine down the outside of the tube (‘bypassing‘), rather than in it. Wet clothing or bed is pretty much guaranteed at some point if you have a permanently indwelling catheter. Changing catheters on a regular basis and being careful when you get dressed, or transfer in to a chair etc can reduce this, but it is still likely to happen at some point.
A suprapubic catheter requires an operation. An incision is made a few centimetres below the belly button, through to the bladder. A catheter is then passed in to the bladder through this new entry. Instead of urine passing via the traditional urethra, it comes out the front and in to a bag that way. There are a few advantages to this. Primarily, there are generally less infections this way. Also, if the person is sexually active, then it keeps things out of the way. But, it requires an actual operation and people with SPC will still get some infections from time to time. If the catheter gets blocked or kinked, then urine will still get passed, sometimes leaking around the catheter entry site in the belly, sometimes through the urethra. The people who I’ve come across who had SPC have generally preferred them to when they had a urethral catheter, but that’s anecdotal. If you are a long term urethral catheter user, it may be worth a conversation with a doctor, preferably a urologist, about the pros & cons of a SPC, especially if you are, or want to be, sexually active.
Intermittent Self Catheterisation is where we started. This is generally the preferred route for people who are in retention of urine. The catheter is single use, used then disposed of. One is passed each time the person needs to empty their bladder. Because it is sterile when it enters and it doesn’t remain in place, the risk of infection is greatly reduced. In fact, with good technique, the risk is almost zero. Because a catheter is passed, the bladder will empty completely. A bladder not entirely emptying is another significant risk of infection. If the person has good dexterity, then this is generally a simple procedure and my experience of the pee fountain is unusual. Once the bladder is empty, the catheter is disposed of and the person goes about their day once more. For the reasons mentioned earlier, this technique is easier for men to carry out as the end of the urethra is easier to see. If manual dexterity is reduced, then this may not be the ideal way to empty a bladder, although a carer could do it for you. Also, if you are a wheelchair user with limited mobility, it may be a challenge getting to the right bits when sitting in the chair. Again, easier for blokes, but even so… It is probably something that some people will find gets easier as they refine their technique, while for others, it simply never works. While we need to have individualised care that works for us and the lives we live, this is probably the preferred method for emptying a neurogenic bladder. “Neurogenic bladder” is a posh way of saying, one that doesn’t work properly due to nerve damage… which is what we’ve got.
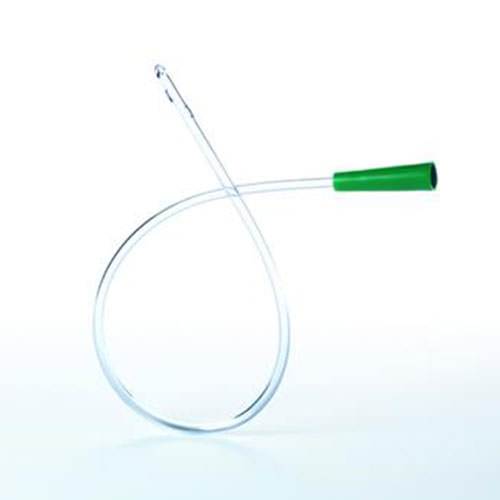
From conveens to catheters, it all appears to be easier if you have a penis. So to make the ladies feel a bit better, I’ll point out that long term indwelling catheters for men can cause a number of other problems including prostate damage (abscesses) so that’s good then… Another reason why ISC is preferred over in-dwelling catheters for long term use.
Then there is, the ‘Crede’s Method‘. This is what I accidentally stumbled across. It is not generally the ‘go to‘ method of emptying a bladder that is in retention for two key reasons.
- It can be difficult to empty the bladder fully. Residual urine is a really, really good way to get some really, really nasty urine infections. If using the Crede’s Method, you really, really need to be able to adequately void the bladder to a point where there is no significant residual urine sitting in the bladder.
- The retained urine can cause the bladder to become over full. If a catheter is inserted (eg ISC), then the urine immediately flows out of the bladder. However, with the Crede’s Method, because pressure is being applied directly to the overly full bladder, urine will pass correctly out of the urethra, while some urine may be forced back up the tubes (ureters) and in to the kidneys. This can result in kidney damage if it happens frequently. This can happen in retention generally, which is why it is a serious condition that requires urgently rectifying.
Now, my Urologist said that in his opinion the kidney damage due to Crede’s Method forcing urine in the wrong direction is “theoretical” and that he’d never come across it in reality. However, he was still concerned about residual urine.
In order to address this, I hit upon my own ‘check’. While through the day, I will visit the toilet as and when I need to, my very last visit to the toilet before going to bed involves me following a routine where I pull myself in to a ‘squatting’ position over the toilet. I then use the Crede’s Method of applying pressure. I now use my stomach muscles to clench/relax/clench/relax to get the urine flowing. I find holding my breath helps. Once the urine is flowing, from the squatting position, I look down between my legs to see the pee.

I’ll then sit down to rest, before repeating.
And repeating.
And repeating.
I continue to cycle through until I don’t see as much as a dribble coming out. Then I can go to bed, safe in the knowledge that my bladder has been completely emptied at least once during the day and no ‘stale urine’ is sitting there breeding bacteria that will cause a UTI.

When I was in rehab and first learning how to do this, the nursing staff were still trying to promote ISC (for all the good reasons mentioned). We agreed that they would do ‘bladder scans’ to see how much residual urine I had after using my method. It was always less than 30ml urine left and frequently the scanner couldn’t detect any. This was seven years ago. My Urologist kept an eye on me for a while, with annual reviews until a couple of years ago when he discharged me. He said at my last review, “keep doing what you are doing, because it is working“. He recommended routine annual blood tests and ultrasound on my kidneys, just to keep an eye on everything, but otherwise, carry on.
Again, bearing in mind the earlier disclaimer, I’m not saying this is the answer for everyone and I’d suggest that if you can, ISC still remains the preferred way to manage a retaining bladder, but discuss things with a professional. Find what works best for you but be aware of the risks too. All methods have some risks, so reduce the likelihood of ‘damage’ as far as possible. If you find that the Crede’s Method works well for you and fits your lifestyle best, then I’d recommend a routine that ensures the bladder is fully empty at least once each day. You will find that many professionals have never heard of Crede’s Method. But then, if you have Cauda Equina Syndrome, you are used to explaining your condition to professionals who’ve never heard of it… …or if you are not, you soon will be!
Now that’s the retention & voiding bit… The joys of the wondrous world of spinal injuries, in particular Cauda Equina Syndrome, is that not content with retaining urine when we want to pee, our bladders will also often choose to empty, or part empty, when we don’t want them to. As a result, wearing a pad is now a life long necessity. I find that I have anything from a maximum of about two minutes, down to twenty seconds of warning, before needing to go to the toilet. If I’m in my house all day, (I’m writing this in July 2020. Due to the COVID-19 pandemic, I’ve been in the house a lot lately!) I can often get through the day with barely a dribble of incontinence. But I still wear a pad ‘just in case‘. Confidence in how my bladder will work, even if I’m not going out, remains very low. In the early days, despite the Crede’s Method and some, albeit short, warning of when I needed to go, I would generally need two pads every day. As well as learning how to ‘empty‘ my bladder, I also needed to re-learn how to ‘manage‘ my bladder. With no sensation for a half or three-quarter full bladder, only ever having a sensation when I get to ‘GO NOW!!!‘ it became something that I needed to think about consciously.
When did I last go? When can I next go?
It is really bad form to refer to adults who have a disability as if they were children. But I’m doing this to myself, so that’s okay…
It was like being a five year old child before going out in the car. The conversation with myself in my head went…
‘Do you need to go to the toilet?‘
‘No‘.
‘Don’t you think you should try?‘
‘No‘
‘Why don’t you give it a go?‘
‘No, I don’t need to‘
‘I really won’t be happy if we have to stop for you to go to the toilet‘
‘Oh alright then! Just stop going on about it!’
Hey! Wadda-ya know? I DID need to pee!
Getting in to a routine of visiting the toilet before going out of the house or workplace etcetera, or going in to a meeting, even if there was no urge to do so, became a big part of managing continence. Thinking ahead, where there may be an accessible toilet? Going to a toilet before leaving a restaurant because you know it is a nice sized, clean environment? Being on the motorway and thinking ‘when did I last go?‘ as you get close to the next service station even when there is no urge… All these help to reduce incontinence. Having a pad helps to give enough confidence not to obsess about toilets. I’ve also noticed behaviour changes, such as, prior to acquiring my disability, if going out, I only ever drank beer. But alcohol is a diuretic, so you pee more (so is caffeine). Beer, being more volume of fluid AND diuretic means visits to the toilet very frequently and still a very wet pad by the end of the evening. Now, I tend to drink wine or shorts more frequently. I’ll still have a beer, but I know there is a price to pay.
And talking of drinking… (this isn’t just thrown together you know… I was working around to this point…)
DRINK PLENTY!!!
It might sound strange but it is important to know, drinking less will cause you to pee more often and increase incontinence. Ideally, drink about three pints of non-alcoholic fluid each day as a minimum. More in hot weather. Cutting down on fluid intake will massively increase the chances of urine infections, which in itself causes incontinence. Going to the toilet frequently and with less time to get there, is often an early sign of a Urinary Tract Infection (UTI). Having a UTI can become very serious and make you quite ill. Also, referring back to the last blog, reducing fluid intake can result in constipation, making bowel management more difficult too. Read it again…
DRINK PLENTY!!!
Night time: My bladder (like other muscles) likes to have a bit of a dance all on its own. At night, it can sometimes have a good ‘spasm’. By contracting, it makes a small amount of fluid feel like a full bladder, which wakes me up. The only way to know if it is full or not, is to try and go. A ‘bad night’ can be anything up to ten times, waking up to try and pee. An average is four. It was actually the disturbed sleep pattern that eventually led to me giving up work, as the fatigue became too much. I have a commode at the side of the bed so I can roll out of bed and on to it, in the dark. If I had to use the actual toilet, I’d need to put the light on, which would wake my wife, so this way I can do it almost half asleep and nine times out of ten, she remains entirely asleep. Also, changing position (lying down) will elevate the legs. This can redistribute fluid, leading to the kidneys firing up and working at a time when the rest of the body is wanting to rest. Some nights I’ll be awake frequently and pass gallons of urine. Other nights, I’ll be awake as often but pass hardly anything, it is just the bladder having a twitch, making it feel that way. There is no pattern to this, although again, alcohol increases the disturbed night as does drinking tea after about 7:30pm.
One random thing that helped is having a ‘smart watch’ that has a torch built in to it. The face of the watch gives out enough light for me to see what I’m doing without putting a light on. It wasn’t a reason for buying the watch, but I wouldn’t be without it now. And it monitors my sleep, so I know how often I get up.
There is a lot more that can be said about urinary continence, but that is beyond what I’m offering here. There are medications that can ‘relax’ a bladder, or botox injections, or surgery… or… or… but these are things that DEFINITELY need to be discussed with a specialist. I have been on medications that reduced the instances of waking during the night. But this blog is aimed mainly at people who are not coping and need some idea about what might be available and why some things are better than others, so not really the place discuss what medication is best… Broken record time, speak to a doctor or continence advisor. Ask for a urology referral. This will give you some ideas about questions to ask. Be an ‘informed patient‘. If things aren’t working for you, ask about alternatives.
And drink plenty of water!
Any questions, feel free to drop me an email keith.fitton@outlook.com
If you came directly here and think the blog is useful, you can subscribe by visiting this page or the HOME page for the menu to other blogs.
Please feel free to comment below, especially if you found it useful or interesting.
Image of ‘Menneken Pis‘ [Flemish for ‘Little Pee Man‘] (c) Mary Warren, on Flickr, kindly used with permission.


